Veteran card players pride themselves on their ability to discern what’s known as “the tell,” a series of involuntary mannerisms that can betray a rival’s strategic deceptions and even suggest a possible next move.
On rare occasions a tell metastasizes into a red flag, a clear indication that something is terribly wrong.
An example of the first is buried deep in a transcript of DaVita Inc.’s annual “Analyst/Investor Day” presentation in New York City.
These meetings were once a love fest for Kent Thiry, the kidney care provider’s colorful chief executive officer, with every year a new opportunity to showcase DaVita’s rapidly expanding earnings per share to an audience of brokerage analysts and portfolio managers. In the fall of 2011 Berkshire Hathaway disclosed it had taken a stake in the company, eventually accumulating just under 38.6 million shares, or 20.2 percent of the company’s public float, perhaps the biggest endorsement a management team can receive.
Shareholders, as the chart below indicates, took a cue from Berkshire and began purchasing DaVita stock hand over fist in the autumn of 2011 at its post stock-split prices in the low $30 range.
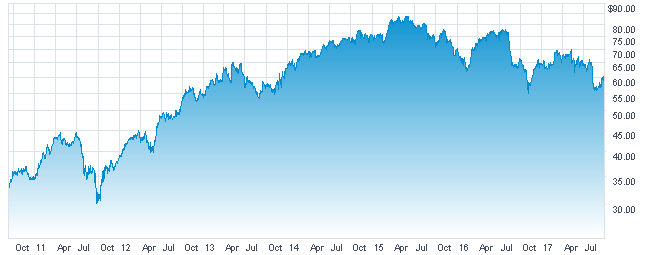
Those meetings are a little less rosy now, however.
At the May meeting, an analyst asked Thiry how much revenue DaVita generates from dialysis patients whose private (more formally known as commercial) health care insurance premiums are paid by the American Kidney Fund’s Health Insurance Payment Program.
Thiry’s response may be studied by future generations of reporters and investors: “We’re not [and] have not and it would not be in your best interest for us to start providing all sorts of detail on that other chunk.”
The Southern Investigative Reporting Foundation, which is attracted to executive prevarication like a large health care corporation is to a dubious insurance billing gambit — and whose interests assuredly lie in exposing undisclosed risk — took Thiry’s non-answer as a challenge.
After all, a limelight-loving CEO suddenly getting cold feet when asked a basic question about revenue breakdown is a pretty clear “tell” that whatever the answer is, it can’t be too good.
The answer looks terrible for DaVita’s investors. The company’s finances, according to a Southern Investigative Reporting Foundation accounting analysis, appear to be massively levered to an opaque nonprofit, the American Kidney Fund, that may provide up to half of its operating profits. They should define HIPP as a “gravy train,” albeit one perhaps soon to be modified by the word “imperiled” as a combination of civil litigation and regulatory shift poses an existential threat to this cozy relationship.
————————
The definition of HIPP is unusually subjective, depending largely on whether you provide or receive dialysis, or insure those who undergo it.
To the former, the AKF and dialysis clinics — especially the larger chains — it’s an elegant solution to an end-stage renal disease conundrum of longstanding: With the one-two punch of its steep financial costs and the physical exhaustion emerging from treatment, working is often not an option, and many patients exhaust savings or go deeply into debt to maintain their private health care insurance policies. As a function of that, AKF’s HIPP pays its recipients monthly insurance premiums for the duration of their dialysis treatment.
For the latter, mostly insurance companies offering health care to the public, HIPP is a financial headache of a scale eclipsed only by its sheer evil brilliance.
They argue that in the AKF, dialysis providers created a low-risk gambit that exploits a narrow Department of Health and Human Services provision allowing third parties — that is, themselves — to donate hundreds of millions of dollars tax-free to the AKF. The fund then enrolls patients (primarily from its largest donors) who receive the same quality of dialysis care at the same providers alongside Medicare patients. But because a small segment of patients have HIPP, the dialysis providers — two of whom control almost three-fourths of the market — can bill insurers many times the roughly $250 per treatment that Medicare will pay.
Using DaVita’s Securities and Exchange Commission filings, the AKF’s Internal Revenue Service annual Form 990 filings and a little extrapolation, the Southern Investigative Reporting Foundation estimates that at a minimum, AKF’s support helps generate between 40 percent and 45 percent of the Kidney Care unit’s estimated earnings before interest and taxes, or at least $339.4 million through June 30, after a one-time $526.8 million legal settlement with the Veterans Affairs Department is backed out of its results. For 2016, it was more than $728.5 million.
(DaVita has two units: Kidney Care, providing patient dialysis and related lab services, and DaVita Medical Group, which owns physician practices. The Kidney Care unit’s earnings, given DaVita Medical Group’s consistent losses, are thus the company’s profits.)
What makes the AKF’s role so astounding is that those handsome profits come from a base of about 9,000 dialysis patients, barely more than 4 percent of DaVita’s 194,600 patients.
Last October, in response to insurer outrage over skyrocketing dialysis reimbursement levels on commercial policies purchased from the Affordable Care Act’s Health Insurance Marketplace, DaVita announced that it would no longer support patient applications for AKF premium assistance on those policies.
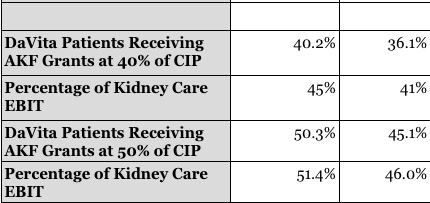
Where DaVita’s own figures weren’t available, conservative assumptions were made, like pegging the growth rate of dialysis patients — historically 3.8 percent — at 1.9 percent through June 30. Given that over 78 percent of the AKF’s $309.8 million in donations last year came from either DaVita or Fresenius Medical Care, the German medical conglomerate that is its primary competitor in dialysis services, the Southern Investigative Reporting Foundation estimated that at least 40 percent of the AKF’s HIPP grants went to DaVita patients.
(Both DaVita and the AKF declined to answer the Southern Investigative Reporting Foundation’s on the number of HIPP recipients receiving dialysis in its clinics, but based on interviews with executives at rival dialysis providers the 40 percent figure was deemed “very conservative.”)
DaVita, in its 2016 Capital Markets presentation, disclosed that privately insured patients are between 110 percent and 115 percent of the Kidney Care unit’s earnings before interest and taxes. To obtain the value of the AKF’s premium support to the company’s profitability, the quotient of the AKF’s commercially insured patients and the company’s commercially insured patients was multiplied by 113 percent.
Seen narrowly, given Thiry’s ownership of more than 2.54 million shares, refusing to discuss the question of AKF’s value to DaVita certainly served his “best interests.” Similarly, as an 18-year veteran of these presentations, he is surely aware that portfolio managers, trained to value a company based on a multiple of its future earnings per share, rarely pay 17 times earnings for a company whose profit growth is slowing and where 40 percent of the operating profit is dependent upon a charity and its circular donor scheme.
Another way to read Thiry’s reticence is as a function of the fact that the AKF relationship is — in the parlance of value investors — DaVita’s sole moat, or a sustainable economic advantage separating it from competitors.
DaVita is an unusual addition to Berkshire Hathaway’s portfolio because its moat isn’t a function of managerial acumen, such as GEICO’s efficiencies (which drive its lower-costs), or the pricing power resulting from global recognition of the Coca-Cola brand. The AKF relationship is a loophole, in the purest sense of the word, made fully legal as the result of a 1997 Department of Health and Human Services advisory opinion permitting donations to the AKF from the major dialysis providers.
Ted Wechsler, an investment manager at Berkshire Hathaway overseeing about $10 billion, didn’t discuss the AKF relationship when he elaborated on his thinking about owning DaVita to CNBC in March 2014.
Ironically, one of Berkshire’s leading lights was blunt with his contempt when offering an assessment of a much higher-profile insurance premium payment gambit at Valeant Pharmaceuticals International during a May 2016 Fox Business News interview.
Charlie Munger, Berkshire’s 93-year-old vice chairman, who has long been a student of what he calls the psychology of human misjudgment, said, “The main thing that Valeant did that was unbelievably clever was to pay the consumers part of the deductible for the drugs they were selling. . . . They paid the consumer share of the deductible and tried to pretend that it was a charitable contribution, when really it was the functional equivalent of bribing the other fellow’s purchasing agent.”
It’s not clear if Munger thinks the AKF is “unbelievably clever” also since he didn’t respond to a request for comment at publication time, but the carve out enabling donations to the AKF did two very important things: It appeared to seal off the fund and the so-called large dialysis organizations — then, as now, primarily DaVita and Fresenius — from prospective kickback allegations. It also enabled both companies to reap the fruits of their multiyear roll-up of competitors.
In a nutshell, insurance companies are required to offer dialysis coverage under network adequacy standards. This is no small matter given that the U.S. government annually spends an estimated $34 billion on dialysis suggesting that commercial insurers — often about 12 percent of the dialysis pool — may spend up to another $5 billion.
The consolidation of dialysis providers and the proliferation of commercial health insurance payors means that in most markets, a patient with end-stage renal disease in need of dialysis might only have DaVita and Fresenius to choose from, affording the company an unusually strong negotiating position.
So how favorable were the deals? The 2017 Medicare base payment for one dialysis treatment is $231.55, although a $250 “blended rate” that takes into account the Medicare Advantage program is likely closer to actual payment levels. For 2016, brokerage analysts estimated that DaVita’s received $1,050 per treatment from commercially insured patients. Even with 88 percent of their patients on Medicare or Medicaid, blended revenue of $346.98 (per treatment) through June 30 led to a 27.4 percent EBITDA margin.
Remarks from Thiry in January at the J.P. Morgan health care conference in San Francisco shed light on how some of these commercial contracts came to be so lucrative.
In a word: outlier contracts.
Seemingly unaware the microphone was still running, at about the 23 minutes 20 seconds point Thiry said that a few commercial insurers this year became aware that their dialysis contracts were so far above market that they chose “to do dramatic things” and “crash and burn” rather than quietly renegotiate. Fortunately, he said, “we’ve had those kinds of contracts for 17 years” and that there “are still a few” of these sharply above market contracts in place.

Having a few outlier contracts in force adds up, and quickly: Assuming three dialysis treatments a week for one patient, that $8oo daily differential between commercial and government reimbursement becomes $9,600 in a month and over a year, $115,200.
DaVita’s business imperative thus becomes simplicity itself: obtain as many commercially insured patients as possible, a plan congruent with its insistence that at current Medicare rates they lose money on 88 percent of their patients.
Enter the AKF.
As gambits go, the AKF relationship is tactically a stroke of genius: the donations to the foundation are tax-free and given an estimated break-even threshold of $250 per dialysis treatment, DaVita’s ability to collect over $1,000 per session generates a heroic return on its capital.
The connection between the HIPP program remaining in effect exactly as it is and the happiness of DaVita shareholders is essentially the union of two sets — should HIPP be curtailed, or a hard cap of two or three times the Medicare rate be placed on commercial insurance payments, its investors could see earnings per share cut in half.
What’s remarkable about this daisy chain is that the AKF only has one condition to satisfy. In the 1997 opinion, the HHS stipulated that the AKF had to make the HIPP program available to qualified patients with end-stage renal disease, and as part of the evaluation process, were forbidden from using the level of support given the foundation by the patient’s dialysis provider as a criteria.
A growing chorus of voices, however, are alleging that the AKF has not lived up to this obligation.
A New York Times investigation last December described social workers at independent and smaller dialysis organizations as having difficulty in obtaining AKF grants for their dialysis patients. In several instances, according to the Times, social workers said that their patients weren’t eligible for HIPP because of their clinic’s inability to donate.
Additionally, a St. Louis Post-Dispatch story last October cited internal DaVita emails in which dialysis clinic-based social workers appear to have been prompted to steer dialysis patients to commercial insurance policies, away from Medicare and Medicaid.
The relationship between DaVita and the AKF prompted the U.S. Attorney for the District of Massachusetts to issue a subpoena to the company in January.
Dr. Teri Browne, a professor at the University of South Carolina’s College of Social Work, told the Southern Investigative Reporting Foundation that as a 10-year veteran of clinic-based nephrology social work for Fresenius and Gambro Healthcare (a company DaVita purchased in 2004), that DaVita patients were encouraged to leave government insurance for commercial plans solely to improve dialysis revenues. In her view, she felt that this was distorting the mission of the social workers to deliver the best information for the dialysis patient.
(Last September, in response to a Centers for Medicare & Medicaid Services request for Information from end-stage renal disease stakeholders on whether patients were being inappropriately steered to Marketplace plans, Browne filed this statement alleging that this practice was occurring on a regular basis, especially at large dialysis organizations.)
Referring to the current debate over whether DaVita is using donations to the AKF to boost its revenues, Dr. Browne said that as she interpreted it, “The 1997 [HHS] ruling was originally written to help people with the supplemental charges in Medicare and Medicaid plans.” She noted, “Based on what I from interviewing dialysis patients, and what my email listserv [of nephrology social workers] is discussing daily, steering patients away from Medicare is now a closely tracked part of their business.”
And “no one is saying that the AKF or its policies are all bad,” she said, “but [the fund] is [incentivized] to expand clinic-centered dialysis. The large dialysis organizations, who give the fund most of its money, are the obvious beneficiaries.”
Asked what the biggest concern she has with the state of dialysis today, Browne argued that dialysis patients switching to private plans from Medicare/Medicaid are often put at major financial risk should they get a transplant. (The AKF’s premium assistance doesn’t cover transplants.)
“Higher premiums and co-pays are the patient’s obligation if they get a transplant,” said Dr. Browne, who added “patients can harm their listing eligibility for transplants by switching.”
Both the AKF and DaVita have strongly denied, to the Southern Investigative Reporting Foundation and other press organizations, any linkage whatsoever between donations and HIPP enrollment. The AKF said it has taken a series of steps to clarify its policies rejecting any quid pro quo, and it submitted this statement to the CMS last September in defense of its practices.
DaVita’s Thiry, in a Sept. 17 question-and-answer session at a R.W. Baird conference, defended premium assistance as functioning exactly as intended, with everything “totally above board,” while acknowledging “[HIPP is] precipitating quite a political football.”
Thiry also used the R.W. Baird conference as an opportunity to defend the broader concept of switching to commercial insurance, describing the coverage offered dialysis patients as being “vastly superior” to Medicare/Medicaid. (There is no data to suggest that private payers have any better clinical outcomes with dialysis than those on Medicare or Medicaid.)
DialysisPPO, a Malvern, Pennsylvania, dialysis consultancy that offers insurance plan and third-party administrators guidance in reducing dialysis costs, published a November 2016 white paper that argued a line broadly supportive of dialysis provider practices:
“When you lose money on 75% of your volume, you have to make extraordinary profits on the remaining minority. On average, our clients are charged 2,100% of the Medicare allowable amount for the same services. The average monthly charges for each [end stage renal disease] patient is $67,000 across our client-base. It is not unusual for monthly dialysis charges to exceed $85,000.”
Sarah Summer, associate general counsel and director of state policy for Blue Shield of California, took the opposite tack in this interview, claiming that “inappropriate third party payments” via AKF HIPP grants were part of “fraud gaming abuse” imperiling the health of insurers in the ACA Marketplace. Her arguments were amplified in Blue Shield’s Request for Information filing last September. Elaborating on the massive costs the San Francisco-based insurer alleges are shifted upon them, its statement described dialysis providers as using the AKF for “payment arbitrage” to capture up to $170,000 in payments per patient.
Blue Shield of California also stated that the burden of HIPP costs make it nearly impossible to remain economically vital: “Assuming a one percent operating margin for Blue Shield, it takes 3,800 members enrolled for 12 months to make up for a single dialysis patient enrolled by the American Kidney Fund.”
Notwithstanding the very real complexity of treating kidney failure, the fact of the matter is that DaVita made over $1.8 billion last year and its filings show that it hasn’t seen a sub-25 percent operating margin in ages. Those profits, common sense would suggest, come from its ability to push prices ever northward. The New England Journal of Medicine’s Catalyst blog, in an article in June, referenced a 2012 study from a trio of healthcare economists who, in analyzing the effect of competition on the quality of dialysis care for the National Bureau of Economic Research, found that’s pretty much what’s going on.
According to these economists, “average spending for DaVita and Fresenius patients rose about 50% from 2005 to 2009, to about $120,000 annually. Spending for dialysis patients in Medicare rose about 20% during that time, but reached only about $60,000 a year.”
More importantly, statistically speaking it doesn’t seem to matter who pays for treatments since U.S.-based dialysis patients face odds that are measurably slimmer than their peers across the globe. According to the University of California San Francisco’s Schools of Pharmacy and Medicine’s Kidney Project, as many as 25 percent of U.S. dialysis patients die in the first year of treatment, and only 35 percent survive as long as five years. The figures are even more stark when compared to a five year mortality rate of three percent for transplant patients.
————————
The commercial insurers are not sitting on their hands and have taken to the courts to begin the work of pressing their interests, which mostly center around filling in DaVita’s moat.
The first shots were fired in a lawsuit filed last July when UnitedHealthcare of Florida sued DaVita competitor American Renal Associates.
Given that UnitedHealthcare’s primary line of legal attack is to frame the relationship between American Renal Associates and the AKF’s HIPP as a dubious “pay to play scheme” designed only to drive dialysis provider profits and not improve lives, the possible implications for DaVita and its interests are clear.
UnitedHealthcare alleges that the AKF’s administration of HIPP left little to the imagination about how little the fund adhered to the intent of the 1997 Department of Health and Human Services ruling, pointing to its “HIPP Honor System” whereby in the event dialysis providers were unable to “make fair and equitable contributions [to the AKF], we respectfully request that your organization not refer patients to the HIPP program.”
Through last autumn, UnitedHealthcare alleges in an exhibit attached to a filing made in June, this policy allegedly connecting HIPP grants to dialysis provider contributions was posted on the AKFs website.
Aetna is taking a different approach to addressing its costs from the AKF’s HIPP grants, at least for now. In April, it sued DaVita in Pennsylvania’s Montgomery County Court of Common Pleas to enforce what it claims are provisions in its contract with the company that allow it to examine data related to AKF HIPP grants awarded to Aetna members.
DaVita, naturally, disagreed that the contract has that provision and claimed that Aetna hadn’t followed the proper dispute resolution procedures. On the second-quarter conference call in May, Javier Rodriguez, the DaVita executive who runs its Kidney Care unit, told analysts that Aetna’s request was denied.
This isn’t the full picture of where things stand between Aetna and DaVita, though.
A Montgomery County judge rejected the emergency component of Aetna’s request but the balance of its litigation was left to proceed, a state of affairs Rodriguez termed “working with Aetna.”
————————
Spokeswomen for both the AKF and DaVita declined to make executives available for phone interviews but provided written replies to emailed questions. DaVita was provided with the model used to determine the connection between AKF HIPP grants and its profitability, as well as the clip of Thiry talking at the J.P. Morgan conference. While dismissive of the Southern Investigative Reporting Foundation’s questions as biased, a spokeswoman declined requests to elaborate on what, if anything, was incorrect.
Corrections: The original version of this story carried an incorrect number for DaVita’s U.S. patients. According to the company’s third-quarter 10-Q, it is 194,600 not 214,700. Additionally, a reference to a published report that provided an inaccurate estimate of the combined Fresenius and DaVita market share was deleted.
Old news – where were you 6 months ago?
Would it be much different if you accept donation from Jim Chano and write a short report so your donors can profit thanks to the action of your “nonprofit” organization? Maybe you shall interview the patient who are dying, whether they benefit from AKF. Maybe it’s the insurance companies who are too greedy. When is the last time that your prescription bills/treatment Not being rejected by insurance companies as “un-necessary”?
The following statement can easily be proven to be unequivocally false: “The company’s finances, according to a Southern Investigative Reporting Foundation accounting analysis, appear to be massively levered to an opaque non-profit, the American Kidney Fund, that may provide up to half of its operating profits.”
The AKF’s IRS 990 (http://www.kidneyfund.org/assets/pdf/about-us/akf-990-2016.pdf) shows $309 million of total grants paid in 2016, a figure that is even cited in the article. Let’s be wildly conservative for the sake of argument and assume 100% of that money is paid to DVA at 100% margin. At $1.3 billion of LTM net income, DVA would still have $1.0 billion of net income if AKC went away entirely. More realistically, 40% of AKF contributions go towards DVA treatments at a 75% margin (50% post-tax). This works out to $62 million of net income from AKF, or 5% of total. This does not even back out the expense of any charitable contributions paid by DVA to AKF.
Yes, huge margins from the relatively smaller segment of privately insured patients subsidize small losses from the relatively larger segment of Medicare patients. But there is no evidence here that the profitability from privately insured patients is in any meaningful way dependent upon the AKF.
Chris, you are misunderstanding the dynamics. AKF provides support to pay the cost (say $400 a month) for a commercial insurance policy. DaVita then bills *that insurer* for dialysis services. So $400 per month in “support” converts a government-pay patient providing $6,000 per month in revenue to a private-pay patient providing $18,000+ per month (and apparently as much as $67,000 per month for clients of DialysisPPO). THAT is how $400 in premium assistance turns into an incremental $10,000 or more of profit for DaVita. “Donations” are sent out into the world and, through the magic of the AKF scheme, they pick up thousands of dollars in additional insurance money on their way through the system (which by the way raises the cost of private insurance for everyone). Does that make it clear?
maybe DVA not as bad as being painted here, but seems like a low quality business model to say the least… even if they grow profits, who on earth would pay up for the stock?
16x p/e seems way too rich even if 1/2 this stuff is true… looks like co profits not sustainable absent the commercial insurance subsidy game. how do we even value this LT?
What is most interesting to me is the rise in short interest and spike in options activity just BEFORE this was posted online. Perhaps the SEC will do some investigating of its own
Mike, thanks for your response – that is indeed clear. Why do you think commercial insurers would so vastly underprice those policies? ACA pre-existing condition restrictions didn’t go into effect until 2014. DVA was still very profitable prior to that.
It’s a nice conspiracy theory, but given how much DVA has to lose if the ACA is repealed next week (loss of Medicaid/ACA arbitrage, potential loss of essential health benefits), I imagine it’s just investors placing a wager on the outcome.
But I do agree the SEC should do some investigating. Into DVA that is, not Mr. Boyd.
Megallan, as a dialysis Nurse for Davita for approximately 15yrs and Fresenius for approximately 14 I have seen first hand how aggressive their campaign has been to enroll patients into these plans. I have seen the discrimination to Medicare/medical patients. Private pay patient have the lay of the land in the clinics. There schedules,certain sitting arrangements and so on. Managers and social workers are put on conference calls and list for allowing a commercial/ private pay to leave and any complaints are handled in favor of the private pay. It’s criminal. Tax payers should get better for their money
A couple of reasons. First, dialysis hasn’t historically been very high on the insurance companies’ radar screen for cost reductions — instead they’ve been focused on bigger ticket items such as cancer. Second is that the smaller companies (and even of the some bigger ones) that offered new plans on the ACA exchange didn’t realize how much dialysis “Usual & Customary” charges were. It wasn’t the pre-existing conditions component, it was a failure to negotiate contracts. If you go back through DaVita’s earnings conference calls, you can hear management talking (albeit cryptically) about how the ACA would benefit dialysis providers (translation: “the new plans have no contracts with us so we can charge nearly the full list price, woohoo!”).
In the end, it appears that — like Icarus — DaVita flew a little too close to the sun on this one. This is no surprise since Kent Thiry might have an even bigger ego than Icarus did. It will be interesting to see if they can find a way to bounce back. If I had to guess I’d say they’ll come through — with a big monetary fine and an updated business model that works for shareholders.
I’m not sure if it matters Foster. This article is primarily a compilation of publicly-available information, there’s little if any Material Non-Public Information (“MNPI”) in it. I don’t think trading with advance knowledge of an article being published is illegal unless the article contains MNPI, but I’m not positive about that. Does anyone here know if it would be problematic, and if so can you point us to the regulation?
So if I understand you correctly then one should stop “Warren and Charlie’s gambit” by shutting down the AKF immediately, which puts DVA into a tailspin due to the significantly reduced EBITDA that will ensure it trips some of its debt covenants. You compromise 40 odd percent of your dialysis clinics in one stroke and my guess is the 10% loss making DVA clinics in rural areas and the inner cities will probably be the first ones to go. Oh and lets not forget the 98,000 patients on HIPP and their families that might have a few issues on top of their weekly dialysis visits to contend with. I recall something about a means and liquid assets test to qualify for HIPP, so they’re probably on it for good reason. That way the insurance companies can breath a sigh of relief, Jimmy boy has his payday and your non profit will probably land a donation or two, totally unexpected of course. Sounds like a plan boys.
Very easy to criticise, but a totally different matter to come up with a workable solution to the terrible diabetes driven epidemic the US is experiencing. You can sling mud as much as you want, but there is no escaping the fact. Someone will pay for these people (let’s not think of them as family, ex coworkers or neighbours) or you let them die. Try dribbling that past your local politician.
My suggestion, if you have the guts to do it, even better ask Jimmy boy to do it; print out your short thesis, head down to your local dialysis clinic (preferably a DVA one) and see what the patients think. Speak to the people that matter.
what I really wants to know if it is true because I can take the lost and move on
Cancer care is the same. Shoddy care for medicare/Medicaid patients. Old toxic chemos for those without private insurance. Trust me very sickening when your loved one is at the mercy of the for profit medical industrial.
Your article failed to cite the recent CMS webinar which directed navigators to direct patients to Medicare and away from the exchanges. This is an important indication of where CMS’ thinking is at today. — https://insidehealthpolicy.com/daily-news/cms-navigator-training-includes-shifting-esrd-patients-medicare
Aside from getting less attention in the clinics (and elsewhere per comments above), does a ESRD or other dialysis patient on Medicare/Medicaid receive a different treatment plan than private – number of treatments, drugs used, etc?
If everyone was on Medicare/Medicaid or some equivalent plan and the cost of dialysis were at the lower rate, could any dialysis business financially survive while paying for good employees (nurses & doctors) and maintain a clean and safe environment for its patients?
Also, some more detail on how Medicare/Medicaid (CMS) sets it rates for dialysis would be helpful. It is possible the problem could be that the government’s payments are too low vs. commercial being too high.
There are a couple of gaping holes here:
1) The author doesn’t highlight the fact that CMS actually benefits dramatically from the imbalance between commercial and Medicare/Medicaid reimbursement rates for dialysis. In effect, commercial insurers are subsidizing CMS patients, to which I say: WELCOME TO AMERICAN HEALTHCARE; THAT’S THE WAY IT USUALLY WORKS. Does anyone really believe that CMS dialysis rates would remain the same if the AKF patients were immediately transferred to Medicare? Ditto for a TON of expensive inpatient hospital treatments, by the way— the same dynamic prevails. The author ignore the fact that CMS creates these distortions in the first place by establishing artificially low, unprofitable rates…
2) There’s an implicit assumption that commercial payors shouldn’t pay for dialysis treatment. Yes, dialysis is very expensive. Isn’t that what insurance is for? If I’m healthy and pay commercial premiums 95% of my life, why should I suddenly be shifted to Medicare/Medicaid when my kidneys fail?
3) The right outcome, imho? CMS rates move up, commercial rates move down.
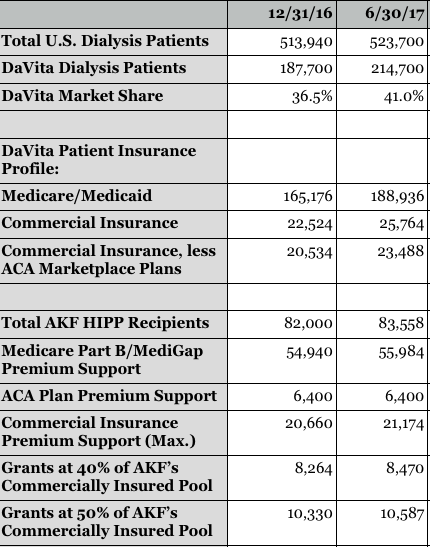
You probably know this, but the numbers in your table is incorrect.
DaVita’s US dialysis patients on 6/30/17 is not 214,700 those are global numbers. You will notice this if you read properly where they quote the above number on their website http://investors.davita.com/corporate-profile
Also, the US patient number is repeatedly quoted 10Q, website, press releases etc as 194,600 https://www.davita.com/about
It can also not easily escape you that your market share number is wrong, because for anyone that studies the industry it is well known that Fresenius and DaVita controls 70% of the industry and have virtually the same market share. Therefore it seems unlikely that you would not have known that the 41% market share number in your table was wrong when the incorrect 214,700 number above “tripped” you up.
I’m waiting for the correction (not holding my breath though).
Jack, “…THE WAY IT USUALLY WORKS” is precisely the problem with “AMERICAN HEALTHCARE.” Regardless of your views, the system is structurally broken, in large part because of gambits such as this one (DaVita is hardly alone among dialysis providers, as noted, for abusive conduct towards the U.S. taxpayer, nor are dialysis providers the worst within the healthcare system.) That said, because a certain kind of conduct has been tolerated in no way means it’s legal or even within the spirit of the law.
Martin, sneer much?
A 9.3% differential, from a company as reticent in providing details as this one, sure got your dander up. I’m happy to make the correction though.
I’d have thought you’d demand a correction about the model’s biggest problem, by far: I’d estimated that about 40%, maybe as much as 45% of pre-tax income was derived from the AKF.
Actually, it’s over 50%.
“You don’t want to know the answer,” indeed.
https://ton.twitter.com/i/ton/data/dm/917736704647270404/917736632312266754/TXMpCdbd.jpg:large
C’mon Roddy you clearly set the tone with your article so don’t complain when people undercut your thesis by pointing out glaring mistakes in your numbers.
I think at the end of the day you will gain more respect by owning up to your errors asap by correcting your numbers and thereby refining your analysis. Otherwise you’re just another guy with an opinion. So let’s start with that correction?
Martin,
The correction was made and an italicized Editor’s Note attached to the top of the article, as is our policy. Additionally, I tweeted the correction in a pair of tweets to draw reader attention to it.
https://twitter.com/RodBoydILM/status/920001362187956225
https://twitter.com/RodBoydILM/status/920001113931345921
There’s a lot of bad behavior in US healthcare — the reporting is interesting here. It will take me more time to digest.
– – – –
I think the TITLE and a couple of Berkshire comments badly miss the mark, though. Simple back of the envelope math refutes the idea the Davita is remotely material to Berkshire.
Fact (1): BRK own many assets and equites are a small portion of that.
Fact (2): I lazily looked at the equity portfolio from end of last year and year before and see it is >$100Bn.
Fact(3): Davita has a market cap of ~$10Bn.
If BRK owned 50% of DaVita (they own much less, in the neighborhood of 20%), then it would still not be material to BRK’s equity portfolio, let alone their company. Typically 5% is a threshold for materiality. DaVita is considerably less than 5% of the equity portfolio, period.
It may be a material investment for the small portfolios run by Todd &/ or Ted. But Warren and Charlie? Impossible.
This is on so many levels (particularly materiality and size does matter a LOT) different from a Ackman-Valeant or Sequoia-Valeant scenario.
A more accurate title to this article would be “An excellent gambit that does nothing material whatsoever for and hence is irrelevant to Warren and Charlie.” We can wordsmith the prepositions as needed.
Back of the envelope calculations in this vein are vital in finance, but for whatever reason, not done much.